Rural vs urban nursing

www.degreechoices.com is an advertising-supported site. Featured or trusted partner programs and all school search, finder, or match results are for schools that compensate us. This compensation does not influence our school rankings, resource guides, or other editorially-independent information published on this site.
Nurses can pursue countless opportunities after graduation, in both small-town and big-city settings. Each location comes with benefits and challenges that may be a better fit for one nurse over another.
- Urban nurses work in cities, towns, suburbs, and large metropolitan areas.
- Rural nurses work in areas with less than 2,500 people or fewer than 500 people per square mile.
- Frontier nurses work in areas that are considered isolated and remote due to either distance in miles or travel time to key services.
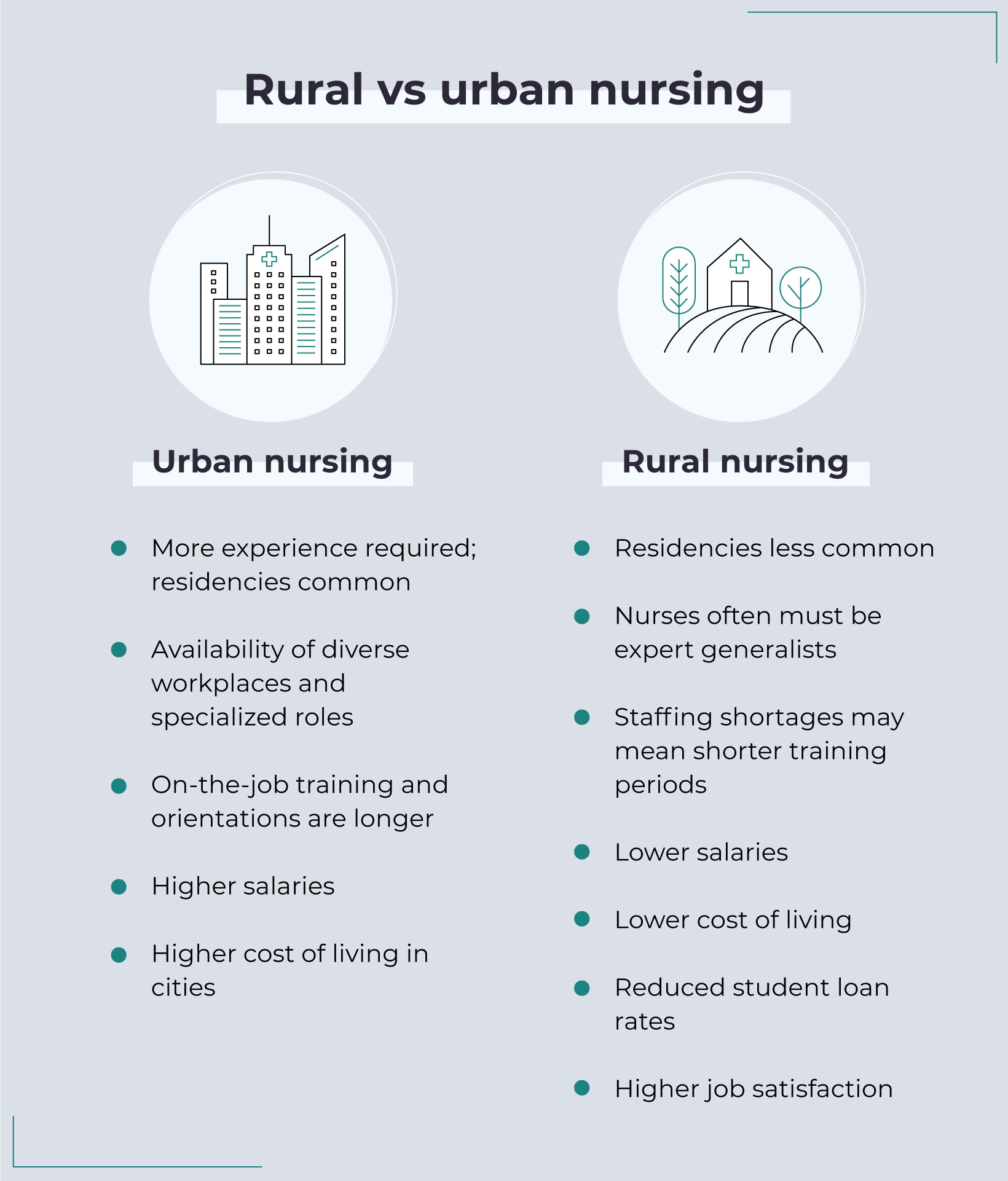
Educational requirements for rural and urban nurses
Both urban and rural nurses must obtain an associate or bachelor’s degree in nursing before sitting for the National Council Licensure Examination (NCLEX exam). Once a new graduate nurse has passed the NCLEX, they can apply for a nursing position. On-the-job training is an important component of nursing jobs – in both rural and big-city settings; however, rural nursing jobs may require less experience.
» Read: Our field guide to nursing
Popular accredited online nursing programs
www.degreechoices.com is an advertising-supported site. Featured or trusted partner programs and all school search, finder, or match results are for schools that compensate us. This compensation does not influence our school rankings, resource guides, or other editorially-independent information published on this site.
Do rural nurses get paid more?
The hourly wage for nurses varies widely across the country and depends on the specific location. Metropolitan hospitals in urban areas are typically better funded, which allows for higher salaries. With additional funding, urban areas can work to retain nurses by offering more competitive insurance, benefits, and pay. Large institutions are also more likely to leverage sign-on bonuses to attract talent to their facility. On the other hand, big cities have a much higher cost of living, which may force urban nurses to live far from their workplace. Some small-town nurses in wealthy states may earn more than urban nurses in low-income areas.
» Read: Your guide to cheap nursing schools
One of the challenges of nursing in rural areas is effectively retaining nurses. Although rural nursing jobs may offer lower pay, additional incentives have been implemented through policy changes and legislation. Examples of these benefits include federal funding to expand nursing school access and reducing student loan rates. In addition to scholarships, some rural hospitals offer student loan repayment options and aim to increase their benefits packages to balance out lower wages.
While rural nurses generally take home smaller salaries, some areas are exceptions, with nurses in Alaska earning similar wages to nurses in large cities.
Urban nurse: average salary
$77,070 – $155,230
Rural nurse: average salary
$30,780 – $71,020
The work environment for rural nurses
Nurses in urban locations can choose to work in various settings, including competing large hospital systems, clinics, urgent care centers, outpatient surgeries, schools, and public health agencies. City jobs are considered fast paced and innovative, as urban hospitals typically have access to the newest technology and offer good remuneration.
Roles are equally diverse, and nurses can become residents, nurse practitioners, physician’s assistants, and ancillary staff such as respiratory therapists and laboratory technicians.
Nurses in rural areas may work in smaller community hospitals, clinics, schools, urgent care centers, and government agencies. Generally speaking though, rural nursing jobs offer fewer workplace options. Many rural communities are drastically underserved, with limited or no access to healthcare.
Some rural locations do not have a physician, which leaves only a nurse practitioner to see patients. Other locations might have several different healthcare providers, but not an abundance of ancillary staff. Due to staffing problems, rural nurses may be at home while on call, whereas nurses in urban areas are more likely to be in the hospital.
Despite these challenges, rural nurses report higher job satisfaction than nurses in large metro areas.
KEY TAKEAWAY
Rural nurses have less access to specialist job positions and diverse work environments, but they report higher job satisfaction.
Orientation and on-the-job training for urban vs rural nurses
Orientation in an urban setting is typically longer and more structured, with a focus on a specialty such as pediatrics, oncology, or labor and delivery. The high volume of specific patient populations allows for the repeated practice of nursing skills to build expertise. Specialty certifications may be required before starting a job or may need to be obtained within a certain period after being hired. New nurses might have access to several different preceptors (aka teachers/mentors) during the orientation process.
» Read: Acing your nursing school interview
Rural nursing orientation can be dramatically shorter, as the hospital unit may be short-staffed. There is not the same volume of similar patient populations to learn specific skills or care through repetition. Rural nursing jobs are best for generalists; there is a focus on gaining competencies within many different specialties across the patient’s lifespan, as opposed to a singular specialty.
KEY TAKEAWAY
Labor shortages may mean that rural nurses spend less time in training.
Skills and characteristics of rural nurses
Rural and frontier areas have fewer employed nurses, with research indicating that they tend to be “older and less educated employees than those in urban studies.” This results in lower ratios of registered nurses to licensed practical nurses in rural areas. Another study of rural nurses indicated that “younger nurses were unwilling to continue working in environments that limit their ability to hone specialized skills, practice to the full scope of their role, and obtain full-time employment.” They believed that younger nurses’ career goals led them to work in urban areas.
» Read: Healthcare jobs you can do from home
Rural nursing jobs set high expectations that new graduate nurses may not immediately meet. For example, crisis assessments and patient management for illnesses and injuries of varying severity throughout a patient’s lifespan require advanced nursing skills learned over time.
The expectation of cross-discipline assessments creates a challenging work environment, so rural nurses must be quick, adaptable learners. They are expected to be expert generalists and become comfortable with working autonomously and independently, as there may not be many other healthcare providers nearby. They must also be critical thinkers and use their creativity to help patients achieve their best outcomes.
Nurses with emergency room experience are highly sought after in recruitment for rural areas, because their skillset can treat a wide variety of illnesses, trauma, and complications. This is vital for nursing in rural areas.
KEY TAKEAWAY
Rural nurses need to be resourceful generalists who learn quickly and don’t mind taking on a variety of tasks.
What are unique challenges for nursing in rural areas?
While the nursing shortage is a nationwide issue, it has a particularly dramatic effect on rural settings. Isolation, fewer resources, sparser populations, and reduced financial incentives limit recruitment of nurses in rural locations. Nursing units in these areas can be drastically understaffed, which requires asking nurses to work more overtime hours or bringing in travel nurses to meet demands.
As many smaller hospitals function as a general healthcare facility for a wide range of people, patients with a critical illness or other serious conditions are routinely stabilized and then sent to larger tertiary centers for specialty treatment. With fewer healthcare providers, nurses must function more independently and maintain a strong understanding of their state’s nurse practice act to guide their decision-making processes.
Patients in remote or isolated areas are more likely to have chronic illnesses that go untreated for long periods of time. These individuals may not seek treatment until their situation is dire, which can lead them to be transferred to a large hospital even farther from their home for advanced treatment.
KEY TAKEAWAY
Rural areas may face staffing issues, so a nurse’s role is often to stabilize a patient’s condition before sending them to a larger healthcare facility.
Potential solutions to rural healthcare issues
Due to the unique challenges that rural healthcare facilities encounter, solutions must be tailored to nursing in rural areas.
- Nursing programs should familiarize students with the generalist approach needed for success in rural areas. Education beyond medical-surgical basics is a requirement for nurses who wish to work in these settings.
- Nurses who work in remote or isolated areas should aim to join support groups and professional organizations for rural healthcare providers. It’s important to stay connected with other providers who may be encountering similar experiences and challenges. This can ultimately help prevent burnout or professional isolation.
- Continued federal funding and grants for rural and frontier areas is needed to assist in improving the number of providers who work in these locations. Education grants increase the number of people who can attend baccalaureate nursing programs and enable additional technology purchases for these programs. Practice grants incentivize healthcare providers to work in medically underserved communities to help increase access.
- Nursing students should seek out loan forgiveness plans, tuition repayment programs, and scholarships as a way to help reduce or pay off student loan debt.
- Providers should offer flexible work schedules. A 2009 study by Molinari and Monserud found that rural nurses were more satisfied with their jobs when they had flexible work hours that support family lifestyles. Adequate staffing allows for more coverage of shifts and fewer scheduling problems.
Key takeaways
Every new graduate nurse will ultimately have to decide between rural nursing and nursing in a larger town, and it’s important to consider several factors before moving forward.
Urban nursing offers the benefits of increased pay, the ability to work with a specific patient population, career advancement, plentiful resources, and interdisciplinary team members.
Nurses who wish to work in rural areas need to determine whether they have the right temperament for the role. This includes an appreciation for the outdoor lifestyle, a desire to be autonomous and independent, and a willingness to become an expert generalist. Rural nurses have the opportunity to care for patients across all stages of life and gain experience treating a wide range of diseases. The variety and community camaraderie are 2 of the biggest benefits of nursing in rural areas.
www.degreechoices.com is an advertising-supported site. Featured or trusted partner programs and all school search, finder, or match results are for schools that compensate us. This compensation does not influence our school rankings, resource guides, or other editorially-independent information published on this site.





